A Review of the Studies – Part 2
Because the AAP, baby product industry, and media want you to hear only the sensationalized incomplete findings.






Of all the SIDS deaths in Alaska from 1992 to 1997, only one infant death involved an infant sleeping on a safe mattress with a non-drug-using parent (< 1% of total deaths).
– Part 2 – Go to Part 1
B. Gessner et al., “Association Between Sudden Infant Death Syndrome and Prone Sleep Position, Bed Sharing, and Sleeping Outside an Infant Crib in Alaska” Pediatrics (U.S.) 108, no. 4 (Oct 2001): 923-7.
Examination of all 130 SIDS in Alaska between 1992 and 1997.
45% of Alaskan SIDS deaths involved some form of bedsharing, while 35% of Alaskan infants cosleep always and 75% do so sometimes or always. (K. Perham-Hester, “Co-sleeping in Alaska: Data from PRAMS. Executive Session of the Maternal-Infant Mortality Review Committee,” Anchorage, AK; December 1999)
Of all the SIDS deaths in Alaska from 1992 to 1997, only one infant death involved an infant sleeping on a safe mattress with a non-drug-using parent (< 1% of total deaths).






F. Hauck et al., “Sleep Environment and the Risk of Sudden Infant Death Syndrome in an Urban Population: The Chicago Infant Mortality Study”Pediatrics (U.S.) 111, no. 5, part 2 (May 2003): 1207-14.
Data from 260 SIDS cases and 260 controls in Chicago, consisting of 75% black, 31% Latino, and 12% white, are analyzed.
Bed-sharing with one or both parents, in any condition, posed 1.4 times the riskof sleeping alone. This factor was stated to be statistically non-significant. There was no compensation made for those sleeping with an adult under the influence of drugs or alcohol, while other studies show these to be significant risk factors in infant bed sharing.
When other children were in the bed, the cosleeping SIDS risk was 3.6 times the risk of sleeping alone (and remember these deaths are included in counts of cosleeping deaths though the term conjures up sleeping with parents).
Breastfeeding appeared to reduce SIDS to 1/5th the risk; however after accounting for factors of mother’s age, education, marital status, and prenatal care, the strength of the number became statistically insignificant. The factors that are more-typically associated with breastfeeding are the same factors that are associated with lower SIDS rates, but studies have not determined how much of this result extends from breastfeeding itself.






C. McGarvey et al.,“An Eight-Year Study of Risk Factors for SIDS: Bed-Sharing vs. Non Bed-Sharing” Archives of Disease in Childhood(Ireland) epub ahead of time: doi:10.1136/adc.(Oct 2005) .074674
287 SIDS cases and 831 controls between 1994 and 2001 in Ireland are examined for factors associated with bed sharing deaths.
 Bed-sharing death risks are reported to be 3 times greater for low birthweight babies. Other studies point out dangers for young, premature infants as well. These tiny and young infants are less-able to move themselves out of a low-oxygen situation and may not put up as much of a fuss to alert parents.
Bed-sharing death risks are reported to be 3 times greater for low birthweight babies. Other studies point out dangers for young, premature infants as well. These tiny and young infants are less-able to move themselves out of a low-oxygen situation and may not put up as much of a fuss to alert parents.
The bed-sharing death risk was 14 times greater for those with smoking mothers.
There was a doubled risk of death for bed-sharing with non-smokers versus lone sleeping, before any other high-risk behaviors were removed from the statistic — and a new risk factor was discovered in this study:
50% of infants dying while bed-sharing were not in their accustomed sleep arrangement — they and their parents were not accustomed to bed-sharing.
Removing this 50% of impromptu bed-sharers would leave no increased risk for customary, non-smoking bed-sharers.
Bed-sharing deaths decrease with age, and babies bed-sharing over the age of 12 months had less than half the risk of sleep-deaths as those sleeping alone.
Heavy blankets and comforters were found to be a major risk factor.
Breastfeeding bed-sharing infants had half the risk of SIDS of non breastfeeding bed-sharers.








D. Tappin et al., “Bedsharing, Roomsharing, and Sudden Infant Death Syndrome in Scotland: A Case-Control Study” Journal of Pediatrics(Scotland) 147, no. 1 (Jul 2005): 32-7.
123 SIDS and 262 control cases in Scotland between 1996 and 2000 are examined for association between bed-sharing and SIDS. Suffocation deaths are included in the term SIDS here.
Sleeping in a separate room, alone, was associated with over 3 times the riskof SIDS as in the same room with parents.
52% of SIDS infants were reported as sharing a sleep surface at some time during the night of death, but they were not necessarily sleep-sharing at time of death. Actually, only 32% were found sharing the parents’ bed at time of death. Use of this statistic for having co-slept some time during the night of death is often used to make co-sleeping dangers sound higher.
The study does not give a figure, but suggests that heavy bedding, (the weight of bedding or duvet is referred to as “tog”), is a strong factor in SIDS deaths (which would be reported as suffocation deaths in some other studies). The study authors found 81% of bed-sharing deaths relating to heavy comforters/bedding in an earlier study of theirs.
Among those found dead in their parents’ bed at time of death, very few of the parents reported that this was their usual place of sleep; meaning again that for most, bed-sharing was not their accustomed sleep arrangement.
This study reports an increased risk of SIDS for breastfeeding in bed-sharing infants, but many of those were found dead in cribs: not cosleeping at the time of death. I consider this a useless finding. Only the number found cosleeping at time of death would be truly useful. Many of those found dead in cribs may have been unaccustomed to crib sleeping, or too fussy to bed-share (for some health reason); although this is conjecture.
20% of control infants were sharing a sleep surface during a reference sleep.
22% of those found sharing at time of death were sharing a couch.
72% of those bedsharing at time of death were under 11 weeks of age.
As usual, no figure is given for the percentage of SIDS cases that represented bed sharing with a safe parent in a safe adult bed.






T. Person et al., “Cosleeping and Sudden Unexpected Death in Infancy”Archives of Pathology and Laboratory Medicine (U.S.) 126, no. 3 (Mar 2002): 343-5.
This smaller study looked at 56 cases of sudden unexpected infant deaths or SIDS diagnoses from the files of one author doctor in Upstate New York. I find this study valuable to mention in that the circumstances of deaths were well described and delineated and provide a good idea of what can be assumed from untold stories in larger studies.
52% of SIDS were sleeping alone: 34% of all SIDS alone in cribs, 9% of all SIDS alone in adult beds, and 5% on couches.
25% of all SIDS cases were in an adult bed with adult(s), in any condition.
7% of SIDS were cosleeping with an intoxicated adult (on bed or couch).
16% of SIDS were cosleeping on a couch.
7% of SIDS cases were cosleeping with a twin in a crib.
(There is no evidence of twin cosleeping to be of greater risk than separate sleeping. It may be safer, as certain physiological advantages have been documented, but the numbers have not been done. Twins, overall, have double the SIDS of singletons. A study of simultaneous twin SIDS deaths reported 8 out of 41 cases where the twins were cosleeping. Anecdotally, cosleeping is very high among twins.)






R. Scragg, E. Mitchell et al., “Bed Sharing, Smoking, and Alcohol in the Sudden Infant Death Syndrome. New Zealand Cot Death Study Group”British Medical Journal (New Zealand) 307, no. 6915 (Nov 20, 1993): 1312-8.
In New Zealand, for the interval between 1987 and 1990, 393 SIDS cases and 1592 controls were examined.
SIDS risk for last sleep in bed with a mother who smoked was 4.5 times the risk of having a non-smoking mother and not sleep-sharing.
For those with non-smoking mothers who were usually bed sharing in the two weeks before their death the risk of SIDS was 1.7, but for those who were bedsharing during their last sleep, there was no risk at all found. Alcohol usage did not appear to be a risk factor in this study.
Still, the actual location at time of death is not reported. While sleeping with a mother with smoke in her lungs can reasonably increase the risk of death after being removed from bed-sharing, there is no apparent reason why, in the absence of a smoking parent, usual cosleeping should increase death risk outside of the parental bed. We have seen that some studies look at whether bed-sharing SIDS cases are with infants accustomed to cosleeping or not. These report that deaths are most-common in impromptu or unaccustomed bed-sharing situations. Notice in this New Zealand study that a higher rate of SIDS is reported for regular co-sleepers, but not for those cosleeping at the night of death. It appears, as in a few other studies, that there may be a danger factor for infants to be alone in a crib when they are accustomed to the regulation of their parental bedsharers. This factor may confound many risk reports for bed-sharing deaths as it is usual to report based upon where the infant was first placed to sleep, spent most of their last night, or simply what their usual sleep arrangement was, rather than where they were actually found at time of death.
SUFFOCATION ALONE:
N. Scheers, J. Kemp et al., “Where Should Infants Sleep? A Comparison of Risk for Suffocation of Infants Sleeping in Cribs, Adult Beds, and Other Sleeping Locations” Pediatrics (U.S.) 112, no. 4 (Oct 2003): 883-9.
This study attempts to compare infant suffocation trends (suffocation diagnoses only, versus all SIDS) between the 1980’s and the 1990’s. While reports from McKenna and others reveal reasons why true SIDS should be lower when sharing sleep with mother, suffocation accidents in adult beds are higher, as they were in cribs before safety education about crib sleeping became widespread.
Although the great number of variables and complicating factors (most admitted to) prevents solid comparisons, the statistical information can provide much insight into the causes of adult-surface deaths, so I have selected this study to use. 883 cases of infant suffocation reported to the Consumer Products Safety Commission from the 90’s are studied.
Their numbers support a 20 times or more risk for suffocation only deathswhile sleeping in actual adult beds versus crib sleeping. This ratio is based upon an assumption that 18% of all infants are sleeping in adult beds. Yet studies suggest that the numbers of infants cosleeping are higher than this number, and adding those in adult beds without co-sleeping would make the true number even higher. Therefore, this estimate of theirs is likely high. There is also likely some portion of the deaths reported as overlying that were actually SIDS before overlying, making this study’s risk figure even slightly more overestimated. There is no mention as to how many of these involved co-sleeping. It is known from other studies that suffocation deaths are greater in adult beds when no protective parent is present. While SIDS deaths should be lower when cosleeping with mother or other protective adult, suffocation accidents are known to be higher in adult beds, as they were in cribs before safety education about crib sleeping became widespread.
Great praise is made in this report as to the large reductions in crib deaths once various mandatory and voluntary safety standards were imposed and parents were educated in making cribs safer. The suggestion was never made to do the same for family beds; rather it was suggested that any attempts to make adult beds safer should be discouraged as they have “unproven efficacy.”
22% of adult-surface suffocations occurred on sofas.
Over 57% of specified-cause suffocations in actual adult beds were due towedging/entrapment; mostly with wall, headboard, or a bedrail. Bedding, plastic, and overlying are other sources of suffocation.
18% of the adult bed suffocations (remember — not of all SIDS, just among those diagnosed as suffocations) are suggested to be from overlying, although it is well understood that this is likely over-diagnosed; often being selected as the diagnosis based solely upon opinions about cosleeping. Even when an infant is found dead underneath an adult’s body, there is often no means of determining whether the adult overlaid onto the infant after it died because it was no longer a warm, reactive body rather it was non-warm and non-responding; more like a pillow.









PACIFIERS:
A pacifier is, of course, an artificial replacement for the mother’s nipple. Scientists have confirmed in many ways that sucking is an important part of babyhood, in terms of emotional comforting and security, neurological development, pain management, and optimal physiological status. Opportunity for natural sucking is likely one component of the reduced SIDS in breastfeeding, cosleeping infants. It has been shown in studies on preemies that providing artificial means of sucking maintains their physiology far better than having no such opportunity, although it does not provide as much benefit as actual nursing at the breast, when available. It is odd, as most pacifier studies do, to suggest an artificial replacement for something natural without even comparing the benefits of the natural version.






P. Fleming et al., “Pacifier Use and Sudden Infant Death Syndrome: Results from the CESDI/SUDI Case Control Study” Archives of Disease in Childhood (England) 81, no. 2 (Aug 1999): 112-116.
This report was performed using the statistics from the CESDI/SUDI study of 325 SIDS infants in England with 1300 matched controls.
While there was no difference between the incidence of SIDS between those who regularly used a pacifier and those who did not, there was a slight difference in the number of infants found dead with pacifiers vs. controls: 40%vs. 51%.






P. Blair, P. Fleming et al., “Sudden Infant Death Syndrome and Sleeping Position in Pre-Term and Low Birthweight Infants: An Opportunity for Targeted Intervention” Archives of Disease in Childhood (England) epub ahead of time: 10.1136/adc.2004.070391 (May 24 2005).
This report was a closer analysis of the above, using the statistics from the CESDI/SUDI study of 325 SIDS infants in England with 1300 matched controls.
This study demonstrates that when an infant was used to using a pacifier, and then not using a pacifier in their last sleep, the statistical odds of dying without a pacifier when accustomed to using one is 17.5 times the risk of not having a pacifier at all.






So How Many Actually ARE cosleeping?
According to the gathered statistics from available studies:
77% of mothers in Oregon bedshare at least sometimes.35% bedshare usually or always.1
41% of African American babies in St. Louis bedshare.2
13% of U.S. infants bedshare usually or always, 20%share half the time or more, and almost
50% were sharing sometime during the two weeks before the survey.This study admits to under represent the poor, leading to anunderestimation of bedsharing percentages .3
75% of Alaskan infants cosleep sometimes or always.35% do so always.4
50% of Chicago infants were bedsharing on a reference night. 5
46% of infants in England are bed-sharing for at least some time during the night. 30% were found bed-sharing on any given night.6
20% of infants in Scotland were sleep sharing during a reference sleep. The number co-sleeping at least part-time would be greater.7
12% are regularly bedsharing in Canterbury, New Zealand.8
23% in Sweden.9
25% of infants studied in Australasia, Europe, and North America.10
1. M. Lahr et al., “Bedsharing and maternal smoking in a population-based survey of new mothers,” Pediatrics (U.S.) 116, no. 4 (Oct 2005): e530-42.
2. B. Unger et al., “Racial and modifiable risk factors among infants dying suddenly and unexpectedly,”Pediatrics (U.S.) 111, no. 2 (Feb 2003): 127-131.
3. M. Willinger et al., “Trends in Infant Bed Sharing in the United States, 1993-2000. The National Infant Sleep Position Study,” Archives of Pediatric and Adolescent Medicine (U.S.) 157, no. 1 (Jan 2003): 43-49.
4. K. Perham-Hester, “Co-sleeping in Alaska: Data from PRAMS. Executive Session of the Maternal-Infant Mortality Review Committee,” Anchorage, AK; December 1999.
5. F. Hauck et al., “Sleep Environment and the Risk of Sudden Infant Death Syndrome in an Urban Population: The Chicago Infant Mortality Study” Pediatrics (U.S.) 111, no. 5, part 2 (May 2003): 1207-14.
6. P. Blair and H. Ball, “The Prevalence and Characteristics Associated with Parent-Infant Bed-Sharing in England,” Archives of Disease in Childhood (England) 89, no. 12 (Dec2004): 1106-10.
7. D. Tappin et al., “Bedsharing, Roomsharing, and Sudden Infant Death Syndrome in Scotland: A Case-Control Study,” Journal of Pediatrics (Scotland) 147, no. 1 (Jul 2005): 32-7.
8. R. Ford et al., “Changes to infant sleep practices in Canterbury,” New Zealand Medical Journal (New Zealand) 113, no. 1102 (Jan 28, 2000): 8-10.
9. C. Lindgren et al., “Sleeping position, breastfeeding, bedsharing and passive smoking in 3-month0old Swedish infants,” Acta Paediatrica (Sweden) 87, no. 10 (Oct 1998):1028-32.
10 . R. Scragg and E. Mitchell, “Side sleeping position and bed sharing in the sudden infant death syndrome,” Annals of Medicine (New Zealand) 30, no. 4 (Aug 1998): 345-9.
The SIDS/Suffocation Risk Factors for Co-Sleeping:
# Bed sharing not being the accustomed sleep arrangement
# Sofa sleeping
# Smoking parent
# Unsafe space between mattress and headboard or wall
# Prone sleeping
# Parent compromised by drugs or alcohol
# Overly heavy or fluffy bedding
# Sleeping with sibling (for tiny infants) or non-interested
adult
# Sleeping without protective parent in room
GRAPH:
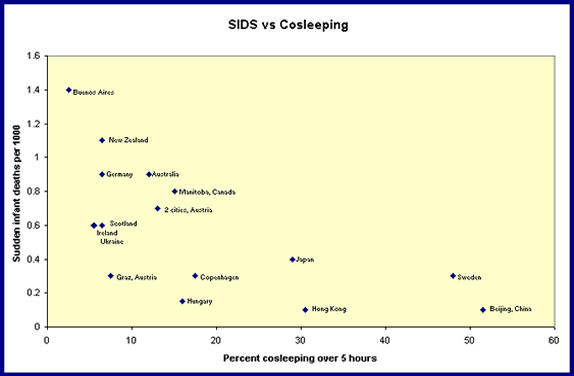
Palmer, 2002. To create the above graph I have taken numbers from the “International Child Care Practices Study ,” Nelson, et al., where data was taken from 17 countries to include 21 centers. The International Child Care Practices Study (ICCPS) has collected descriptive data from 21 centers in 17 countries. The Sudden Infant Death rates for each studied area are plotted against the percent of infants in that area who are cosleeping for over 5 hours per night (percent bed sharing X percent over 5 hours). One more point could be placed at 88% cosleeping for Chongqing, China, with negligible (<.1) SIDS. I have not plotted this point in the graph, as the study authors did not assign an exact SIDS value, and I do not wish to be distorting the graph in favor of conclusions.
The report supplies 1995 statistics. The U.S. was not included. In 1995, the U.S. SIDS rate was 1.0 per thousand. Cosleeping was a little lower than today’s estimated “20% for half the time or more.”
The authors of the study did not propose any graphs. They did not wish to weigh too much conclusion on their study findings as there were many variables, such as fashion of bedsharing and diagnostic criteria for SIDS.
– Part 2 – Go to Part 1


No Comments