I highly recommend that all pregnant mothers become informed about premature infant care. There’s no time to become informed if a premature birth happens to you, and your choices can have huge consequences on the… (continued below)
Newest related post: Fortify Human Milk for Premature Infants?
See also: Should Human Milk Be Fortified For a Premature Baby? and
Preemie Feeding: Human Milk Fortifier? Donor Milk?
For updated information and references, see “BABY POOP.”
By Linda Folden Palmer, DC
2004
I highly recommend that all pregnant mothers become informed about premature infant care. There’s no time to become informed if a premature birth happens to you, and your choices can have huge consequences on the survival and long-term health of your baby. If you’re not informed, medicalization can win out and your baby may lose out – so please do take time to think about the possibilities of preemie care today.
Premature infants present a very special and delicate nutritional case. They are designed to be fed totally processed nutrients in mother’s blood through the umbilical cord; their digestive systems are not well developed, and some may be too weak to suck. Many are given various feeds through tubes, bottles or through needles directly into their veins, even though in other countries all but the tiniest of these infants have been successfully fed by using mother’s milk exclusively.
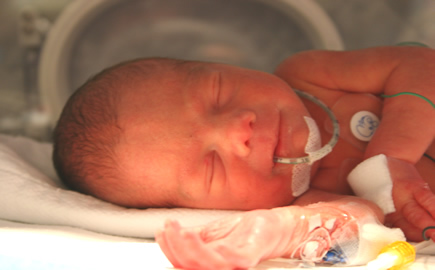
Mother’s Milk is Best
When infants are too tiny or weak for breastfeeding, mothers can express their milk for spoon or cup feeding or for tube feeding if necessary. Artificial nipple (bottle) feeding should not be used in infants intended for breastfeeding because it has been shown to reduce the success of the infants’ continued breastfeeding by nearly two-thirds (known as nipple confusion). Not only does the opioid reward of food intake and sucking help to bond infants to artificial nipples instead of to their mothers’ breasts, but the latching technique, sucking pattern and use of tongue and mouth muscles are very different between bottle nipples and real nipples.
The tiniest infants are generally fed intravenous sugar, fats and protein pieces but can take some breast milk by mouth even on day one. Although seldom practiced in the United States, these infants should be fed on nothing but breast milk as soon as possible — within a few weeks at most.
Nearly all kinds of infections are significantly elevated when premature infants are fed artificial formulas instead of breast milk, including urinary tract infections and diarrheal diseases.
Among the tiniest preemies, there are 45% more serious infections in those exclusively fed formula. While the difference in mortality between low birthweight infants fed breast milk versus formula is not as great as the difference seen between term infant feedings, those not receiving breast milk still have a 26% to 37% greater death rate.
The statistical benefits of breast milk in these studies are reduced by some of the various types of breast milk used (stored, pasteurized, term milk) and the various forms of supplementation or fortification of breast milk. The highest benefit is from fresh premature colostrum and breast milk from the infant’s own mother, although this is not always possible.
Special Benefits for Preemies
It has been found that the preemie’s ability to break down fats from mother’s milk is twice as efficient as from formula. Of course, other nutrients are more available in mother’s milk as well. Many studies on breastfeeding preterm and low birth-weight babies complain that the nutrients in breast milk are lower than in chemically derived milks, and breastfed preemies sometimes gain weight more slowly during their stay in the hospital. However, follow-up studies to age 2 or 3 show there is no difference in the size between naturally or artificially fed babies.
Additionally, studies suggest the breastfed preemie’s growth rate is similar to that inside the uterus. In fact, the bone mineral content is greater in childhood follow-ups in direct proportion to the amount of human milk received. The growth of head circumference, an indicator of brain development, is not lower during premature hospitalization in infants fed human milk, even when the breastfed infant weighs less.
Preterm infants who are fed breast milk grow up with higher intelligence scores, and other neurological development parameters are better as well. Long-term immune development is superior in those who receive breast milk. Breastmilk-fed preterm and low-weight infants have higher survival rates, lower illness rates, stronger bones (eventually), greater intelligence and superior neurological development; hence, weight gain comparisons are not highly relevant.
The Advantages of Warm, Affectionate Care
A big difference in the health of tiny hospitalized infants can be induced by caring for them via kangaroo care and other nurturing measures.
Standard care for Western preemies is to remain in incubators for their first weeks of extra-uterine life. Self-regulation of body temperature is very inadequate in preemies. Temperature, oxygen and infection regulation are the chief purposes of incubators. Of course, breast milk regulates infection, too. It has been found that for all newborns, even very premature infants, placing them skin-to-skin on the chest of the mother or father provides superior temperature regulation to that of an incubator.
Measures of important energy conservation (oxygen consumption) in these infants are excellent as well.
Designed especially for small and preterm babies, “kangaroo care” advocates dressing infants in only a diaper and placing them upright inside the mother’s clothing, in between her breasts.
Here, they can feed or attempt to suckle at will and can enjoy the comfort and gentle stimulation of continued contact with mother — her warmth, sounds and odor. Almost no crying is heard this way, compared to the long pulses of “separation distress calls” normally found in the nursery.
This method of care has become standard in Scandinavian countries (where the infant death rate is half that of the United States) and has been adopted in other European countries for several hours per day. In 1979 in the United States, researchers demonstrated significant improvement in the recovery of newborns when affectionate treatment was given to them on cue.
Not yet ready for allowing the mother in, nurses in the study provided this treatment. Newborns were rocked, cuddled and provided with verbal and visual stimulation and were allowed to suck on a pacifier as much as desired. In comparison to standard care infants, these babies demonstrated superior temperature regulation and respiratory rates; far fewer heart murmurs were detected, fewer sucking and swallowing difficulties were seen and almost no crying was found.
More than 25 years later, some health care practitioners and hospitals in the United States are finally starting to seriously consider this kind of care.
Kangaroo care decreases newborn deaths, and these infants gain twice as much weight per day as standard incubator babies. Kangaroo care also results in more sleep, good oxygen saturation, less agitation, many fewer episodes of apnea (no breathing) and more stable heart rates. A 1999 U.S. school of nursing study confirmed all these findings and reported that kangaroo care would be beneficial for newborns, beginning in the delivery room.
This care can also be used with preterm infants who require tube-feeding; it even accelerates production of a hormone that stimulates secretion of digestive enzymes. Even babies on respirators can benefit from kangaroo care. Hospital stays are much shorter for preemies who receive this kind of attention. This early skin-to-skin care has also been shown to significantly improve mother’s milk volume, a common challenge with preterm births, and it improves mother’s attachment and maternal behaviors.
Oxygenation, temperature control and respiration are all superior when these infants are directly breastfed. Additionally, they have fewer sucking and swallowing problems, they tolerate their oral feedings earlier and their breast milk feedings are greater when received directly at the breast or in another nurturing manner.
When these measures are added, weight gain is faster than for those in standard care. Thus, although a small infant fed breast milk through a tube will have a higher chance of healthy survival than one fed formula by tube, any infant who is fed directly at the breast or who is otherwise fed breast milk with warm body contact and affectionate care will have the best chance for success.
Unfortunately, kangaroo care and exclusive breastfeeding are almost never seen in U.S. neonatal intensive care units (NICUs). Breastfeeding at any level is not always encouraged and sometimes not even allowed. I heard of a mother who was laughed out of the NICU when carrying in one or two tiny ounces of her first colostrum, which is actually “liquid gold.”
I must emphasize that infant mortality rates (up to age 1 year) in the United States are higher than in 41 other industrialized and developing nations who record and report statistics. The restricted availability of premature feeding formulas and supplies, incubators and other equipment in less affluent nations causes premature infants to be more often held and breastfed — hence, they more often survive.
Additionally, it has been shown that early discharge of low-weight infants (at 4 pounds or less), leads to faster weight increases as well as longer breastfeeding with no decline in health or survival rates. In the Philippines, where an infant born at home will generally stay at home regardless of birth weight, low birthweight infants were breastfed far longer when born at home than when born in hospitals.
How to Improve Outcomes
Mothers of underdeveloped infants need to be proactive in order to improve outcomes for their children. Mothers have to be as close as possible to their preemies from the very start to encourage milk production. Just hearing the infant cry will help to promote milk production. When some kind of breastfeeding attempt is made within the first six hours after birth, prolactin levels are much higher than when the first attempts are three days later.
Mothers need to take measures to maintain elevated prolactin levels. If breastfeeding attempts are infrequent or weak, the possibilities include kangaroo care, maintaining nearness to the infant, hearing and responding emotionally to baby’s cries, having the infant attempt to suck or at least nuzzle and regularly attempting to manually express or pump milk (which is beneficial even though only drops may come the first days).
Every time the infant receives food other than mother’s milk, mother’s milk production is impaired. Thus, she should express milk each time such a feeding occurs. It’s important for mother to pump regularly during this period anyway to store milk up that can be given when baby is ready for it and mother is not present.
As mentioned before, many kinds of breast milk are fed to low-weight infants. Pooled donor milk, which is a collection of stored milk from multiple donor mothers, can be of two types: from mothers of term infants or from mothers of premature infants. Mother’s milk after a premature birth is much higher in certain nutrients, and studies show superior growth and head circumference in low-weight infants fed milk from preterm baby mothers.
Important fat absorption is greater when pooled milk is not sterilized. Growth is shown to be even better when mother’s own milk is used, rather than pooled milk, likely because it is fresher and unprocessed, naturally customized to the maturity of the infant and because mother’s exposure to the infant allows her to create customized antibodies in response to the microbes in the infant’s body and environment.
Researchers have just discovered (to their admitted surprise) that when preemies are being bottle-fed or spoon fed, these infants, when allowed, quickly become able to self-regulate their caloric intake when fed in response to hunger and to satisfaction. There are many confirmed advantages to on-cue feeding, especially less frustration and better digestion. There is also less energy expenditure from crying while waiting for feeding. This point is very important in the weak, tiny preemie. In all likelihood baby knows best, yet scheduled feeding of prescribed dosages continues to be the norm in hospitals, likely because they are easier to monitor in this kind of setting.
© Linda Folden Palmer
——————————————————————————–
Resources
R.N. Musoke et al., “Breastfeeding promotion: feeding the low birth weight infant,” Int J Gynaecol Obstet (Kenya) 31, suppl. 1 (1990): 57–9.
G.P. Mathur et al., “Breastfeeding in babies delivered by cesarean section,” Indian Pediatr 30, no. 11 (Nov 1993): 1285–90.
J. Contreras-Lemus J et al., “[Morbidity reduction in preterm newborns fed with milk of their own mothers],” Bol Med Hosp Infant Mex 49, no. 10 (Oct 1992): 671–7.
M.A. Hylander et al., “Human milk feedings and infection among very low birth weight infants,” Pediatrics 102, no. 3 (Sep 1998): E38.
S.P. Srivastava et al., “Mortality patterns in breast versus artificially fed term babies in early infancy: a longitudinal study,” Indian Pediatr 31, no. 11 (Nov 1994): 1393–6.
S. Awasthi et al., “Mortality patterns in breast versus artificially fed term babies in early infancy: a longitudinal study,” Indian Pediatr 28, no. 3 (Mar 1991): 243–8.
M. Armand et al., “Effect of human milk or formula on gastric function and fat digestion in the premature infant,” Pediatr Res 40, no. 3 (Sep 1996): 429–37.
R.J. Schanler et al., “Bone mineralization outcomes in human milk-fed preterm infants,” Pediatr Res 31, no. 6 (Jun 1992): 583–6.
J. Ramasethu et al., “Weight gain in exclusively breastfed preterm infants,” J Trop Pediatr (India) 39, no. 3 (Jun 1993): 152–9.
N.J. Bishop et al., “Early diet of preterm infants and bone mineralization at age five years,” Acta Paediatr (England) 85, no. 2 (Feb 1996): 230–6.
G. Putet et al., “Nutrient balance, energy utilization, and composition of weight gain in very-low-birth-weight infants fed pooled human milk or a preterm formula,” J Pediatr 105, no. 1 (Jul 1984): 79–85.
A. Lucas et al., “A randomised multicentre study of human milk versus formula and later development in preterm infants,” Arch Dis Child Fetal Neonatal Ed (England) 70, no. 2 (Mar 1994): F141–6.
B. Lozoff, “Birth and ‘bonding’ in non-industrial societies,” Dev Med Child Neurol 25, no. 5 (Oct 1983): 595–600.
K. Christensson, “Fathers can effectively achieve heat conservation in healthy newborn infants,” Acta Paediatr (Sweden) 85, no. 11 (Nov 1996): 1354–60.
J Bauer et al., “Metabolic rate and energy balance in very low birth weight infants during kangaroo holding by their mothers and fathers,” J Pediatr (Germany) 129 no. 4 (Oct 1996): 608–11.
K. Christensson et al., “Separation distress call in the human neonate in the absence of maternal body contact,” Acta Paediatr (Sweden) 84, no 5 (May 1995): 468–73.
C.C. Lambesis et al., “Effects of surrogate mothering on physiologic stabilization in transitional newborns,” Birth Defects Orig Artic Ser 15, no. 7 (1979): 201–23.
L. Vaivre-Douret et al., “[Kangaroo method and care],” Arch Pediatr (France) 3, no. 12 (Dec 1996): 1262–9.
R.A. Kambarami et al., “Kangaroo care versus incubator care in the management of well preterm infants — a pilot study,” Ann Trop Paediatr 18, no. 2 (Jun 1998): 81–6.
P.R. Messmer et al., “Effect of kangaroo care on sleep time for neonates,” Pediatr Nurs 23, no. 4 (Jul–Aug 1997): 408–14.
S.M. Ludington-Hoe et al., “Birth-related fatigue in 34–36-week preterm neonates: rapid recovery with very early kangaroo (skin-to-skin) care,” J Obstet Gynecol Neonatal Nurs 28, no. 1 (Jan–Feb 1999): 94–103.
C.J. Tornhage et al., “Plasma somatostatin and cholecystokinin levels in preterm infants during kangaroo care with and without nasogastric tube-feeding,” J Pediatr Endocrinol Metab 11, no. 5 (Sep–Oct 1998): 645–51.
K. Gloppestad, Vard Nord Utveckl Forsk (Norway) 16, no. 1 (spring 1996): 22–7.
N.M. Hurst et al., “Skin-to-skin holding in the neonatal intensive care unit influences maternal milk volume,” J Perinatol 17, no. 3 (May–Jun 1997): 213–7.
P. De Chateau and B. Wiberg, “Long-term effect on mother–infant behavior of extra contact during the first hour post partum. I. First observations at 36 hours,” Acta Paediatr Scand 66, no. 2 (Mar 1977): 137–43.
G. Gale et al., “Skin-to-skin (kangaroo) holding of the intubated premature infant,” Neonatal Netw 12, no. 6 (Sep 1993): 49–57.
M.E. Wegman, “Infant mortality: some international comparisons,” Pediatrics 98, no. 6, part 1 (Dec 1996): 1020–7.
M.J. Martin Puerto et al., “[Early discharge of low-birth-weight neonates. 5-year experience],” An Esp Pediatr (Spain) 38, no. 1 (Jan 1993): 20–4
L.S. Adair et al., “The duration of breast-feeding: How is it affected by biological, sociodemographic, health sector, and food industry factor?” Demography 30, no. 1 (Feb 1993): 63–80.
K. Aisaka et al., “[Effects of mother-infant interaction on maternal milk secretion and dynamics of maternal serum prolactin levels in puerperium],” Nippon Sanka Fujinka Gakkain Zasshi (Japan) 37, no. 5 (May 1985): 713–20.
V. Nedkova and S. Tanchev, “[Serum levels of prolactin, progesterone and estradiol in nursing mothers,]” Akush Ginedol (Solfiia) (Bulgaria) 34, no. 3 (1995): 22–3.
S.J. Gross, “Growth and biochemical response of preterm infants fed human milk or modified infant formula,” N Engl J Med 308, no. 5 (Feb 3 1983): 237–41.
G. Boehm et al., “[Consequences of the composition of breast milk for the nutrition of underweight newborn infants. II. Lipids and lactose],” Kinderarztl Prax (Germany) 57, no. 9 (Sep 1989): 443–50.
Narayanan, “Human milk for low birthweight infants: immunology, nutrition and newer practical technologies,” Acta Paediatr Jpn (Japan) 31, no. 4 (Aug 1989): 455–61.
K. Pridham et al., “The effects of prescribed versus ad libitum feedings and formula caloric density on premature infant dietary intake and weight gain,” Nurs Res 48, no. 2 (Mar–Apr 1999): 86–93.
R.J. Schanler and S.A. Abrams, “Postnatal attainment of intrauterine macromineral accretion rates in low birth weight infants fed fortified human milk,” J Pediatr 126, no. 3 (Mar 1995): 441–7.
S. Awasthi et al., “Is high protein milk beneficial for SGA-terms?” Indian Pediatr 26, no. 1 (Jan 1989): 45–51.
G. Boehm et al., “[Protein utilization by premature infants with a birth weight less than 1,500 g during nutrition with MANSAN or breast milk protein],” Kinderarztl Prax (German) 59, no. 1–2 (Jan–Feb 1991): 26–30.
R. Quan et al., “The effect of nutritional additives on anti-infective factors in human milk,” Clin Pediatr (Phila) 33, no. 6 (Jun 1994): 325–8.
A. Lucas et al., “Randomized outcome trial of human milk fortification and developmental outcome in preterm infants,” Am J Clin Nutr (England) 64, no. 2 (Aug 1996): 142–51.
J. Kreuder et al., “[Efficacy and side effects of differential calcium and phosphate administration in prevention of osteopenia in premature infants],” Monatsschr Kinderheilkd (Germany) 138, no. 11 (Nov 1990): 775–9.
S.J. Gross, “Bone mineralization in preterm infants fed human milk with and without mineral supplementation,” J Pediatr 111, no. 3 (Sep 1987): 450–8.
J. Neuzil et al., “Oxidation of parenteral lipid emulsion by ambient and phototherapy lights: potential toxicity of routine parenteral feeding,” J Pediatr 126, no. 5, part 1 (May 1995): 785–90.
D.A. Kelly, “Liver complications of pediatric parenteral nutrition — epidemiology,” Nutrition 14, no. 1 (Jan 1998): 153–7.
R.L. Fisher, “Hepatobiliary abnormalities associated with total parenteral nutrition,” Gastroenterol Clin North Am 18, no. 3 (Sep 1989): 645–66.
K. Simmer et al., “The use of breast milk in a neonatal unit and its relationship to protein and energy intake and growth,” J Paediatr Child Health 33, no. 1 (Feb 1997): 55–60.
A. Lucas and T.J. Cole, “Breast milk and neonatal necrotising enterocolitis,” Lancet (England) 336, no. 8730 (Dec 1990): 1519–23.
V. Araujo et al., “Impact of oxygen therapy on antioxidant status in newborns,” Biofactors 8, nos. 1–2 (1998): 143–7.
L. Daniels et al., “Selenium status of preterm infants: the effect of postnatal age and method of feeding,” Acta Paediatr 86, no. 3 (Mar 1997) 281–8.

[…] What You Need to Know Now About Feeding A Premature Baby […]